Co-Author: Kendrea L. Focht, Ph.D., C.Sc.D., CCC-SLP, CBIS
Evidence, rather than opinion, should guide clinical decision-making.1
Introduction
The complexity of oropharyngeal swallowing and swallowing impairment mandates an accurate assessment that is grounded in the understanding of the physiologic swallowing mechanism, and is standardized in the protocol, interpretation, reporting, and overall communication across the continuum of care. Value of the physiologic assessment is clear when the results are combined with and related to patient factors such as health, nutrition, and quality of life. Further, the assessment should be sufficiently rigorous in training, practical in execution, and linked to clinical action, specifically to evidence-based, targeted, and individualized treatment. These assessment characteristics and years of experience with attempting to interpret results from clinicians using wide variations in modified barium swallowing study (MBSS) practices underpinned the motivation for the development of the Modified Barium Swallowing Impairment Profile (MBSImP).2 Patients should not have to undergo multiple exams as healthcare providers change because of ambiguous reporting of results between facilities, nor should they experience unnecessary radiation exposures related to prolonged studies that have low clinical diagnostic yield in the attempt to replicate every possible consistency on a patient’s meal tray.
The MBSS is the most commonly used instrumental method for the assessment of oropharyngeal swallowing function by speech-language pathologists (SLPs) and radiologists since it permits indirect visualization of the functional continuum of swallowing in real time.1 The MBSS is a videofluoroscopic procedure designed to permit observations of the rapid, interdependent physiologic motions of oropharyngeal, laryngeal, and cervical esophageal structures relative to bolus flow.3,4 The MBSS also includes observation of esophageal clearance in the upright position because of the evidence supporting associations between oropharyngeal and esophageal function in dysphagic patients.5,6
The MBSImP is a standardized approach to the instruction, assessment, and reporting of swallowing physiology and impairment from off-line observations of videofluoroscopic images obtained during a MBSS.2,7,8 The MBSImP was developed and tested during a five-year supported study by the National Institutes of Health (NIH/NIDCD) in over 300 dysphagic patients (the details of the study are described in the 2008 publication in Dysphagia, and the full-text is available online to the public at http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4217120/) and has been the subject of study for 15 years.2 The purposes of the MBSS and MBSImP approach in adults are to: 1) identify and distinguish type and severity of physiologic swallowing impairment; 2) provide surrogate information regarding sensorimotor mechanisms that contribute to swallowing impairment (e.g., weakness, sensation, etc. that cannot be directly testing but inferred based on evidence); 3) determine the presence, cause, and patient response to airway invasion (penetration/aspiration); and 4) assess the response and adaptations of the mechanism(s) to interventions that identify treatment targets and guide the clinician’s plan of care.2,8
The web-based training program, disseminated by Northern Speech Services (http://www.northernspeech.com/MBSImP/), includes standardized training in swallowing physiology, skill development, and reliability testing (Figure 1).7 Our team worked for 2 years with industrial partners to construct physiologically accurate animations derived from data that reflected each MBSImP score (72 representations) to facilitate training and enhance learning (Figure 2).7 Once clinicians demonstrate reliable scoring, they are permitted to enter de-identified patient demographic data, MBSImP results, patient reported and clinically reported qualitative outcomes, and specific measureable goals (Figure 1).7 The HIPPA compliant, de-identified database includes query functions regarding detailed physiologic recovery and outcomes over time in like patient groups, response(s) to intervention(s), performance improvement data, and also generates automated reports from radial dial entries to import into electronic medical record systems.7 The MBSImP is the first international data record of dysphagic patients that currently houses over 14,000 records. Severity and outcome metrics based on large numbers of dysphagic patients are under development to assist clinicians with converting physiologic and patient reported outcome measures into severity indexes for purposes of patient stratification for clinical research and billing documentation.
 Figure 1. MBSImP web-based training program and database by Northern Speech Services (available at http://www.northernspeech.com/MBSImP/).
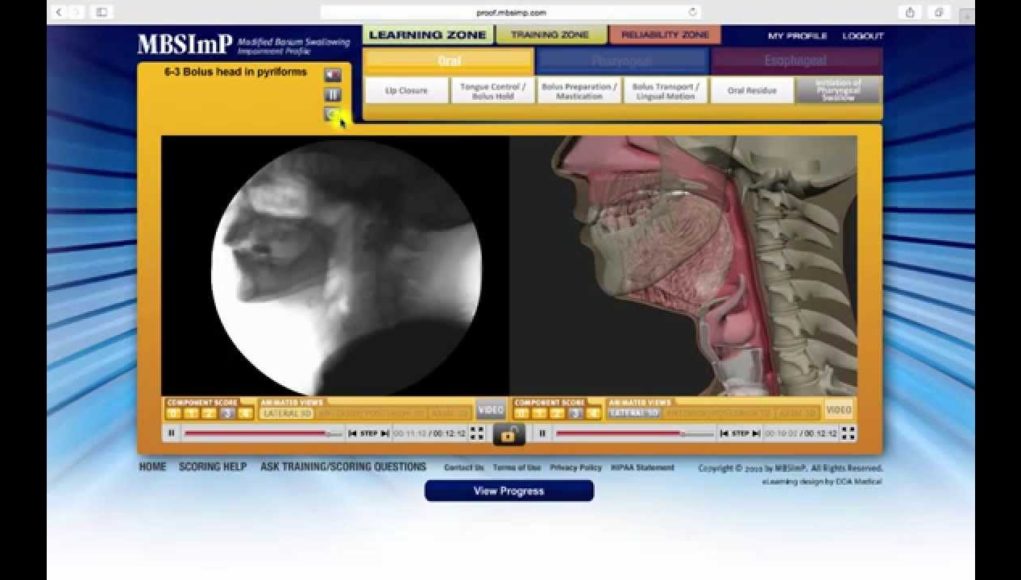
Figure 1. MBSImP web-based training program and database by Northern Speech Services (available at http://www.northernspeech.com/MBSImP/).  Figure 2. Example of videofluoroscopic and 3-D animated images during MBSImP online learning.
Figure 2. Example of videofluoroscopic and 3-D animated images during MBSImP online learning.
Importance of standardization when providing patient care
In general, standardized practices in health care have been shown to facilitate patient safety, continuity of patient care, unambiguous reporting and interpretation of results, and improved clinical outcome.1 Specialized and standardized training that includes accuracy and reliability of measurement, and the standardized execution of the evaluation and interpretation are required to optimize the diagnostic result.
The goal of the MBSS is to determine the physiologic cause of airway invasion to serve as the focus of targeted intervention or restoration.8
Swallowing is no different than any other test of physiologic function. In fact, one could argue that the results acquired by inadequately prepared clinicians and poorly executed MBSSs could lead to dire patient outcomes that interfere with pulmonary health, nutrition, and significantly impact the overall health and well being of patients. The MBSImP is an evidence-based approach that is Patient-Centered as opposed to Clinician-Centered (i.e. “this is what I expect from this exam” versus “this is how I like to do it/this is how I have always done it”). Wide variations in clinical practice place patients at increased risk. The purpose of the MBSS is to assess the patient’s physiologic mechanism using a standardized set of safe, tailored contrast materials based on longstanding evidence that simulate a range of volumes and tasks that include liquids, semisolids, and solids that lead to informed and accurate clinical decisions regarding intake status and/or nature of oral intake.2,9,10 The MBSS is not an assessment of feeding; feeding assessment requires controlling variables such as environmental factors, supervision, fatigue, etc.8 It is not possible to conduct a thorough feeding assessment in a few minutes while exposing the patient to radiation. Thus, a trained clinician is able to judge how the swallowing mechanism will adapt to interventions without introducing multiple trials of unstandardized materials during the MBSS, which can be observed from follow-up observations during mealtime or therapeutic feeding sessions.
Using the MBSImP approach, varied volumes and viscosities are tested in a selective way since evidence supports the existence of modification in oropharyngeal and esophageal physiology using standardized contrast (barium) materials. In countries where standardized materials are not available, clinicians trained in the MBSImP approach are working toward internal consistency for the contrast materials that are administered during the MBSS to optimize reliability and validity of test results.
Every attempt should also be made to standardize radiographic data acquisition, recording, and viewing planes (lateral and anterior-posterior views).2,7,8 The clinician should practice diligence to take the necessary, but reasonable steps to capture the swallowing continuum from the lips through the esophagus. The fluoroscopic equipment needs to be capable of continuous fluoroscopy or 30 pulses per second.8 Previous work from our lab has demonstrated fluoroscopy settings and recording rates influence the details necessary for accurate assessment of swallowing physiology that subsequently influence treatment decisions.11 When clinicians are trained using the MBSImP approach, average fluoroscopy exposure is under 3 minutes, which includes implementing compensatory strategies and swallowing maneuvers.12
Clinicians must improve their confidence in MBSS execution and results by optimizing their understanding of the swallowing mechanism and how it adapts to various bolus types and swallowing tasks. This confidence and understanding is enhanced when implementing a systematic approach and avoids the emphasis of the evaluation away from the presence or absence of aspiration (albeit important information that is an integral part of the MBSS further discussed below).
Physiologic components of swallowing
The MBSImP assesses 17 physiologic components of swallowing impairment derived from evidence available in the scientific literature and through expert consensus of a panel of 13 internationally recognized specialists in the field of swallowing and swallowing disorders.2 The 17 components were grouped across 3 functional domains of swallowing, and each component uniquely contributes to judgments of overall swallowing impairment.2,7,8 The Oral Domain includes components related to oral containment, oral tongue motility, and oral bolus clearance.2,7,8 The Pharyngeal Domain comprises components related to airway protection and pharyngeal bolus clearance. 2,7,8 The Esophageal Domain includes one component – esophageal bolus clearance in the upright clearance – that falls in the scope of practice of SLPs. 2,7,8 A trained clinician is able to capture impairment by observing components across bolus volumes/consistencies to formulate an overall impression score for each swallowing component.2,7,8 The MBSImP was also designed to capture impairment even when all swallowing trials are not possible during the MBSS (e.g., patient safety, physician order).2,7,8
Oral Domain
- Lip closure
- Tongue control during bolus hold
- Bolus preparation/mastication
- Bolus transport/lingual motion
- Oral residue
- Initiation of pharyngeal swallow
Pharyngeal Domain
- Soft palate elevation
- Laryngeal elevation
- Anterior hyoid excursion
- Epiglottic movement
- Laryngeal vestibular closure
- Pharyngeal stripping wave
- Pharyngeal contraction
- Pharyngoesophageal segment opening
- Tongue base retraction
- Pharyngeal residue
Esophageal Domain
- Esophageal clearance in upright position
These physiologic components have been and continue to be tested for their association with other important factors, such as general health, oral intake, nutritional status, and quality-of-life.2 Past and new evidence support the relevance of MBSImP component scores to the swallowing function of the patient. Large cohorts of patients, careful research, and multivariate statistical analysis are required to execute such studies that are ongoing in our laboratories.
Comment about aspiration
The MBSS is not a “pass or fail test” based on the presence or absence of aspiration (i.e., entry of ingested material into the airway).8 Aspiration is neither a necessary or sufficient measure of swallowing impairment since impairment can exist without accompanying aspiration observed during a MBSS.8 The goal of the MBSS is to determine the physiologic cause of airway invasion to serve as the focus of targeted intervention or restoration.8 Since scores are not including in the MBSImP scoring metrics, it is recommended that validated Penetration-Aspiration Scale (PAS)13 be used in conjunction with the MBSImP to capture this information regarding swallowing safety and should be evaluated in tandem.1,7,8
Conclusion
To date, approximately 3,000 clinicians and 5,000 graduate students are currently enrolled in the MBSImP online training program. Trained and registered users are located in all 50 states in the United States, 10 provinces in Canada, and 17 additional countries around the world. Graduate speech-language pathology programs using the MBSImP in their dysphagia courses reached 80 in 2014. Evaluation of oropharyngeal swallowing physiology should be conducted by like-trained clinicians with similar specialty training and credentials from programs with standardized curriculums that include rigorous competency assessment. The MBSImP is a standardized approach to instruction, assessment, and reporting of physiologic swallowing impairment based on observations during a MBSS – all of which are necessary to capture and communicate the complex process that occur during normal and impaired swallowing.
About the Authors
Bonnie Martin-Harris, Ph.D., CCC-SLP, BCS-S, ASHA Fellow is Professor in the Department of Otolaryngology-Head and Neck Surgery in the College of Medicine and in the Department of Health Sciences and Research in the College of Health Professions at the Medical University of South Carolina (MUSC). She is Director of the MUSC Evelyn Trammell Institute for Voice and Swallowing. She also serves as Director of the doctoral program in Health and Rehabilitation Science at MUSC. Currently, she is the Associate Editor for the Dysphagia journal and previously served as Associate Editor for the Journal of Speech-Language-Hearing Research. She is a past-President of the Dysphagia Research Society and past Chair of the Specialty Board on Swallowing and Swallowing Disorders (BCS-S). Her research has previously and currently is funded by the National Institutes on Deafness and Other Communication Disorders (NIH/NIDCD) and Veterans Affairs (VA RR&D).
Disclosures: MBSImP research and development was funded in part by NIH/NIDCD, Bracco Diagnostics, and the Mark and Evelyn Trammell Foundation. Dr. Martin-Harris also receives royalties and speaking fees from Northern Speech Services. She receives a salary from MUSC, and currently receives grant funding from NIH/NIDCD and the VA.
Kendrea L. Focht, Ph.D., C.Sc.D., CCC-SLP, CBIS is a Research Health Scientist at the Ralph H. Johnson Veterans Affairs Medical Center and a Post-Doctoral Fellow in the Department of Otolaryngology-Head and Neck Surgery in the College of Medicine at the Medical University of South Carolina (MUSC). She is also a Speech-Language Pathologist (SLP) at the MUSC Evelyn Trammell Institute for Voice and Swallowing. Her research is currently funded by the Veterans Affairs (VA RR&D).
Disclosures: Dr. Focht receives a salary from MUSC and the Medical University Hospital Authority. The VA currently funds her research.
References
- Agency for health quality research. Translating research into practice (TRIP)-II. Fact sheet. Rockville, MD; 2001.
- Martin-Harris B, Michel Y, Brodsky MB, et al. MBS Measurement Tool of Swallow Impairment—MBSImp: Establishing a Standard. Dysphagia. 2008;23:392-405.
- Logemann JA. Manual for the videofluorographic study of swallowing. 2nd ed. Austin, TX: PRO-ED, Inc.; 1993.
- Logemann JA. Evaluation and treatment of swallowing disorders. 2nd ed. Austin, TX: PRO-ED, Inc.; 1998.
- Gullung J, Hill EG, Castell DO, Martin-Harris B. Oropharyngeal and esophageal swallowing impairment: Association and predictive value of Modified Barium Swallow Impairment ProfileTM© and combined multichannel intraluminal impedence-esophageal manometry. Ann Oto Rhinol Laryngol. 2012;121(11):738-745.
- Allen JE, White C, Leonard R, Belafsky PC. Comparison of esophageal screen findings on videofluoroscopy with full esophagram results. Head Neck. 2012;34(2):264-269.
- Northern Speech Services. Modified Barium Swallow Impairment Profile. https://www.mbsimp.com. Accessed February 4, 2015.
- Martin-Harris B. Standardized training in swallowing physiology: evidence-based assessment using the Modified Barium Swallowing Impairment Profile approach. Gaylord, MI: Northern Speech Services, Inc; In press.
- Logemann JA, Gensler G,…,Miller Gardner PJ. A randomized study of three interventions for aspiration of thin liquids in patients with dementia or Parkinson’s disease. J Speech Lang Hear Res. 2008;51(1):173- 183.
- Robbins J, Gensler G,…Miller Gardner PJ. Comparison of 2 interventions for liquid aspiration on pneumonia incidence: a randomized trial. Ann Intern Med. 2008;148(7):509-518.
- Bonilha HS, Blair J Carnes B, Huda W, Humphries K, McGrattan K, Michel Y, Martin-Harris B. Preliminary investigation of the effect of pulse rate on judgments of swallowing impairment and treatment recommendations. Dysphagia. 2013;28(4):528-538.
- Bonilha HS, Humphries, K, Blair J, Hill EG, McGrattan K, Carnes B, Huda W, Martin-Harris B. Radiation exposure time during MBSS: influence of swallowing impairment severity, medical diagnosis, clinician experience, and standardized protocol use. Dysphagia. 2013;28(1):77-85.
- Rosenbek JC, Robbins JA, Roecker EB, Coyle JL, Wood JL. A penetration-aspiration scale. Dysphagia. 1996;11:93-98.