With contributions from: Maribel Ciampitti, MS, CCC-SLP and Gail Sudderth, RRT
Introduction
By the year 2020, there will be over 600,000 patients requiring prolonged mechanical ventilation.1 Many of these patients will have dysphagia and require the interventions of a speech-language pathologist (SLP). There is a paucity of research regarding best practices for managing this challenging population. Patients receiving mechanical ventilation are often complex cases. They have multiple medical comorbidities that require intense medical management but also contribute to swallowing impairment. Therefore, the timing and nature of swallowing therapy should be considered in the context of the patient’s overall medical goals and interventions. Dikeman and colleagues wisely described the close collaboration that is needed among the entire medical team as a “juggling act”, one that balances the patient’s pulmonary needs and interventions for other disordered clinical systems (i.e. central nervous, cardiac, and renal) with clinical goals such as weaning and return to oral intake.2 Although it is impossible to develop a strict step-by-step or “cookbook” approach, the following guidelines and principles are offered based on the available evidence. A case study is also presented to exemplify this approach.
Use It or Lose It
Many clinicians believe it is necessary to wait until the patient is weaned from mechanical ventilation to begin dysphagia intervention. Sometimes there is an impression that the patient is too sick. However, evidence indicates that a delay in treatment may do more harm than good. Up to 50% of intensive care unit patients who require ventilation present with Systemic Inflammatory Response Syndrome, and 50%-70% of these patients go on to develop diffuse pathological muscle weakness (myopathy) and peripheral nerve disorders.3 Muscle weakness is an independent predictor of pharyngeal dysfunction as well as symptomatic aspiration. Patients with muscle weakness struggle to feed themselves, have greatly reduced cough strength, and poor control over their swallowing and upper airways.4 Furthermore, pneumonia caused by aspiration causes acute lung injury, weaning failure, delayed hospital discharge, and mortality.5
…it is important to first restore the system to its most “normal” and ideal condition, that is, “reconnect” the upper and lower airways. It would be ineffective to begin interventions such as laryngeal exercises or respiratory strength training without adequate airflow, pressure and sensation.
In the physical therapy field, improved outcomes have been achieved with early mobilization of ICU patients.6 Burkhead and colleagues point out that the same principles that strengthen bodies can help improve function of the mouth and throat muscles.7 Therefore, SLPs should provide “physical therapy” to the upper airway early in recovery which can then reduce the effect of muscle atrophy and improve swallowing function. Even if it is unsafe to initiate oral intake, indirect swallowing therapy should be initiated; which can include oral, pharyngeal, laryngeal or respiratory muscle exercises, airway protection and cough strengthening activities, and management of oral secretions.
Make the Connection
Tracheostomy creates a “disconnect” between the upper and lower airways, which results in aphonia, disrupted laryngeal and pharyngeal sensation, loss of subglottic airflow and pressure, reduced smell and taste, reduced cough strength and inability to expectorate secretions. Therefore, to most effectively evaluate and treat swallowing in these patients, it is important to first restore the system to its most “normal” and ideal condition, that is, “reconnect” the upper and lower airways. It would be ineffective to begin interventions such as laryngeal exercises or respiratory strength training without adequate airflow, pressure and sensation. When a patient is still on a mechanical ventilator, this is most optimally achieved through cuff deflation and placement of a Passy Muir® Valve in-line with the ventilator circuit.3
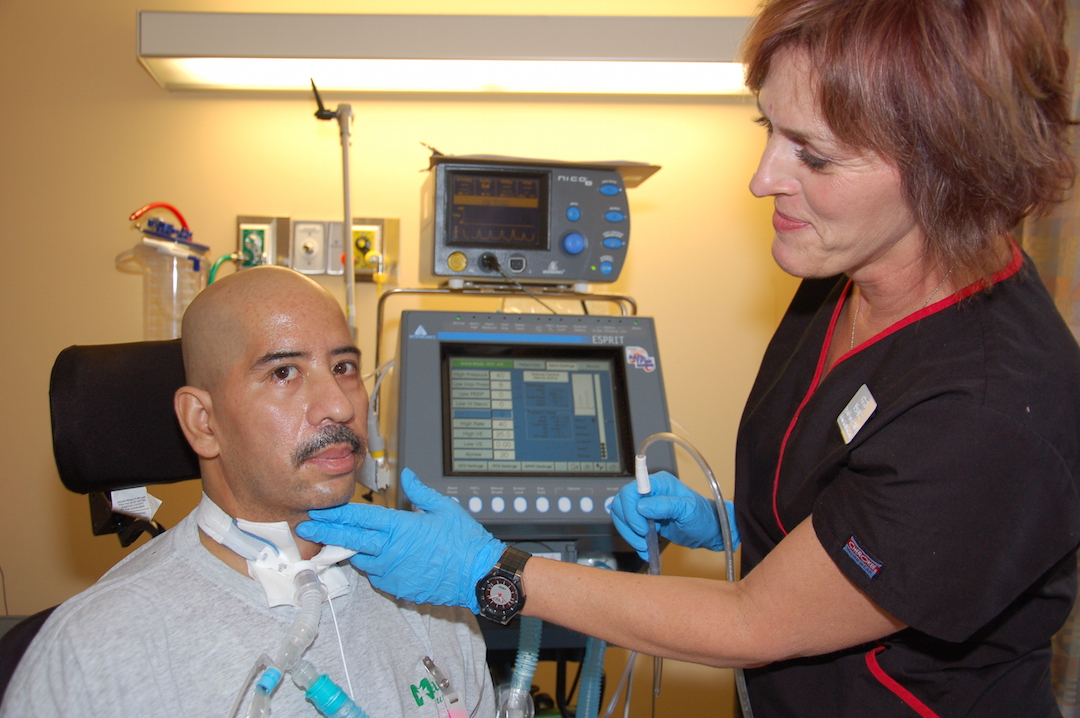
Team Up
In order to “reconnect” the system, assistance from the respiratory care practitioner (RCP) is required. Positive outcomes, including reductions in cannulation times, hospital length of stay, adverse events and cost of care have been realized when patients with tracheostomy are managed with a multi-disciplinary team approach.8-10 For the ventilated patient, the RCP is responsible for procedures including cuff deflation, downsizing the tracheostomy tube, adjustments to the ventilator settings and placement of the Passy Muir Valve in the ventilator circuit.
Hands Down, Cuff Down
Multiple studies have demonstrated that there are higher rates of aspiration when patients have inflated tracheostomy cuffs versus deflated.11-14 In instances when cuffs are overly inflated, swallowing has been shown to be difficult to elicit and slower.15 If a clinical evaluation of swallowing is conducted with an inflated cuff, important signs of aspiration are lost such as coughing, wet vocal quality, visual presence of aspirated material in tube, and the patient’s sensation of material “sticking” in throat.
It is not uncommon, however, that the SLP meets resistance from physicians and RCPs when requesting cuff deflation. There is still the misconception that the cuff prevents aspiration. There is also a fear that adequate ventilation cannot be achieved. The SLP can provide education and evidence to alleviate these concerns. It has been demonstrated that ventilation and stable respiratory parameters can be achieved with the cuff fully deflated16-17 and with placement of a Passy Muir Valve18-21. Most recently, clinicians in a cardio-thoracic ICU were also was able to reveal that deflating the cuff and using the Passy Muir increased end expiratory lung impedance, therefore serving as a lung recruitment intervention.19 Due to these findings, use of Passy Muir Valves with ventilator patients increased from 0% to 70% and is now the standard of care in that ICU. A multi-site ICU study in Spain has also shown a decrease in respiratory infection rates for dysphagia patients using Passy Muir Valves in-line.22
For Trach Tubes, Size Does Matter
Along with cuff deflation, an appropriately sized tracheostomy tube is critical to “reconnecting” the airway. A tracheostomy tube that fills the trachea prohibits airflow through the upper airway and placement of the speaking valve. Unfortunately, guidelines for tracheostomy tube sizing are lacking and many hospitals place the same larger diameter tubes in all patients. Additionally, some facilities wait two weeks or longer to downsize the trach tube. Downsizing the tube, within a week of the tracheotomy procedure, can result in earlier use of a speaking valve, improved swallowing, earlier oral intake, shortened weaning time and reduced length of stay.23-25 Therefore, the SLP should be advocating for smaller tubes early in recovery, if not during initial trach tube placement.
Speaking Valves – Not Just for Speaking
Passy Muir Valve placement restores laryngeal and pharyngeal sensation by directing airflow back through the upper airway instead of the ventilator circuit. Improved sensation enables the opening and closing laryngeal reflexes to return to normal, which restores the protective cough reflex, and contributes to a safe swallow.26-27 Using the valve facilitates exhalation through the upper airway after swallowing which helps to expel material that may be misdirected to the trachea during swallowing.28 And, a reconnected system restores subglottic air pressures which enables patients to achieve appropriate lung volumes, cough, throat clear, and to use other techniques that require subglottic air pressure such as the supraglottic technique and respiratory muscle strength training.29-31 There is a body of evidence that supports the role of the Passy Muir Valve in reducing tracheal secretions, the need for suctioning32-33 and reducing or eliminating aspiration.27,33-36
Often the SLP and medical team wish to establish specific criteria for ventilator settings and patient parameters to begin dysphagia intervention. For example, they may want a protocol that designates a specific respiratory rate, pressure support or oxygen requirement. It is impossible to establish such specific ventilator criteria because there is so much variability among patients.
Using the Passy Muir Valve in-line may require ventilator adjustments in order to assure patient comfort, safety (appropriate alarms), adequate ventilation and ability of patient to perform speech and swallow tasks. These adjustments are made by the RCP trained in such procedures and under the guidance of the physician. As the team proceeds with cuff deflation and placement of the valve for swallowing therapy, priority must be made toward the goal of the patient being able to demonstrate control of the glottis through voicing, coughing, and secretion control. Only then should initiation of oral intake be considered.
Swallowing- How you Breathe Matters
Often the SLP and medical team wish to establish specific criteria for ventilator settings and patient parameters to begin dysphagia intervention. For example, they may want a protocol that designates a specific respiratory rate, pressure support or oxygen requirement. It is impossible to establish such specific ventilator criteria because there is so much variability among patients. Instead, SLPs need to understand what the level of ventilator support means in relation to the patient’s pulmonary function and overall medical status. Additionally, the SLP must have an appreciation of the effects positive pressure ventilation can have on breathing and swallowing coordination.
In healthy adults, swallows are predominantly initiated after inspiration, followed by expiration and occur at certain lung volumes.37-38 The SLP must work with the RCP to understand how particular ventilator settings and the level of patient control of breathing may impact the patient’s ability to synchronize breathing and swallowing. An additional challenge is factoring many other patient variables into this equation. For example, patients with respiratory insufficiency due to either chronic obstructive pulmonary disease.39-40 or neuromuscular diseases41-42 are known to already have breathing swallowing patterns that deviate from the predominate pattern and have higher risk for aspiration.
Consider the common modes of ventilation:
Assist Control (A/C) mode is one in which each breath is initiated and controlled by the ventilator according to a set rate. The ventilator is providing the majority if not all of the work of breathing. On this mode, a patient may achieve better breath support and higher and consistent lung volumes. Higher lung volumes have been reported to contribute to increased subglottic pressure and safer swallows.43 However, the patient may have difficulty timing the swallow with the ventilator controlled breaths, thereby creating a situation of dyssyncrony, non-preferred breathing-swallowing patterns, and increased risk of aspiration.
Pressure Support (PS) mode is one in which the patient, and not the ventilator, controls the timing of the breath delivery. A patient-initiated breath is supported with additional pressure from the ventilator. This mode is often used during weaning as patients assume more of the work of breathing. The effects on swallowing will differ depending on the patient. A potential benefit to this mode may be that the patient can time the swallow with their breathing. The RCP can further assist respiratory/swallow coordination by making adjustments to ventilator settings, e.g. flow terminating the inspiratory flow to shorten inspiratory time and prolong expiratory time. However, patients may experience difficulty as the work of breathing increases and the act of swallowing food or liquid imposes an additional level of demand. Caution would need to be exhibited in these cases and the length of meal time and volume of oral intake considered.
The effects of positive pressure mechanical ventilation on breathing and swallowing interaction are sparse and only beginning to shed light on this subject.44-48 This highlights the importance of close collaboration between the SLP and the rest of the medical team.
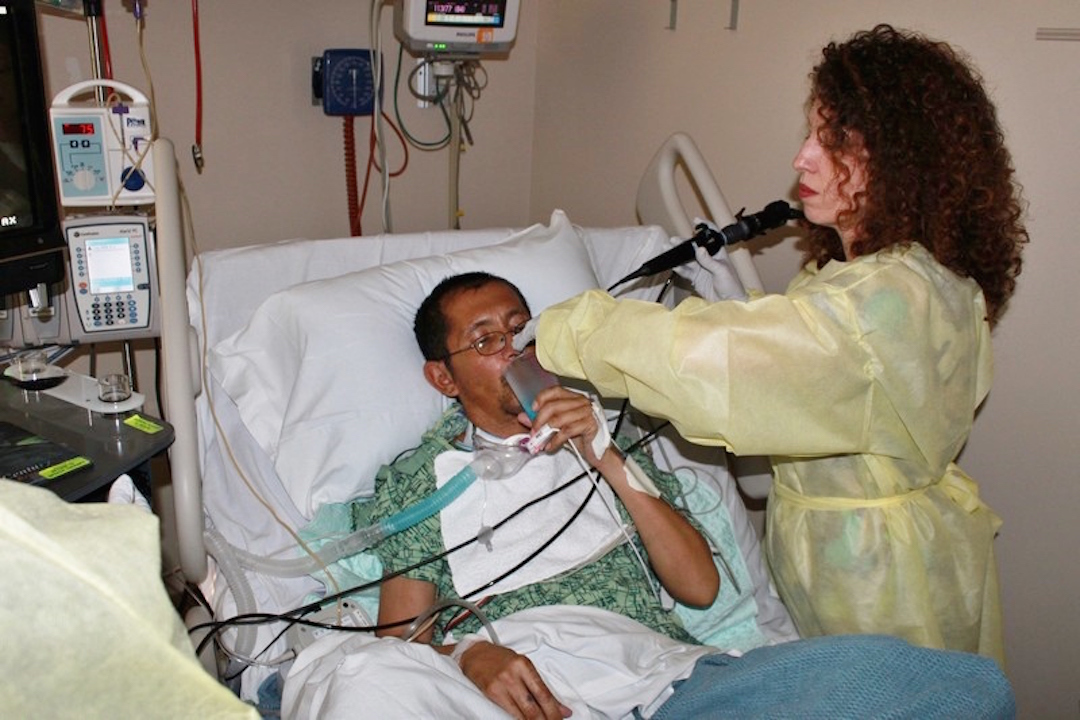
Don’t Be Blue
Incidence of aspiration in patients with tracheostomy is over 50% for patients on ventilators, with a very high frequency of those aspiration events being “silent aspiration”.11,49-50 Clinical studies have indicated that the sensitivity of the modified Evans blue dye method is low (50%) and may yield false negatives.51-54 Therefore, an instrumental swallowing assessment is the only way to document aspiration/silent aspiration. It is the also the most accurate method of assessing the full scope of swallowing function and not just the presence or absence of aspiration.13,34 Whether using videofluoroscopic swallow studies (VFSS) or fiberoptic evaluation of swallowing (FEES), it is advisable to perform the swallowing evaluation under multiple conditions to determine whether the condition is mandatory for a safe swallow3. Evaluation conditions can and should include cuff status, speaking valve use, level of ventilator support, positional and postural changes, and use of facilitative or compensatory strategies.
Putting the Pieces Together- A Case Study
The patient is a 75 year old male admitted to a long term acute care hospital with diagnosis of respiratory failure secondary to severe sepsis related to urinary tract infection, left lower leg wound infection and right lower lobe pneumonia. Patient required tracheostomy and ventilator support.
- Ventilator settings: Assist-Control (AC) Mode, Rate 12, Tidal Volume 400, PEEP 5 cm H2O, and FIO2 .40
- Tracheostomy Tube: Shiley, size 6, cuffed
- Swallow Status: NPO, all nutrition via gastrostomy tube
- Cognitive Status: Confused with periods of agitation. Following some simple commands, nodding yes/no.
- Secretion Status: Copious oral and tracheal secretions, frequent but unproductive cough, suctioning several times per hour.
Week 1:
As a standing order at the treating facility, all tracheostomized and ventilator patients are screened on admission. This patient was identified as a candidate for evaluation by SLP and Passy Muir Valve assessment.
The RCP and SLP collaborated to initiate Passy Muir Valve (PMV) assessment and placement while the patient was on the ventilator in AC mode. The tracheostomy cuff was deflated. It was determined by a drop in pressure and volume that the patient had an adequate leak of air around the trach tube for exhalation. There was no need to downsize the tube. The PMV was placed in the circuit of the ventilator and the RCP adjusted the ventilator to assure adequate volumes and safe alarms. The patient demonstrated audible voice but had persistent wet voice quality and coughing. During this initial session, the patient was cued to clear his throat and cough to mobilize secretions and expectorate them orally. Due to cognitive impairment, he was unable to follow commands for other rehab strategies or exercises. Despite copious secretions and frequent need to cough and expectorate secretions, the patient was able to maintain oxygen saturation, heart rate and respiratory rate within normal limits. As the team continued to wean the patient from the ventilator, the PMV was used 15-30 minutes with supervision to allow the patient opportunities to actively clear secretions and to provide sensory stimulation to the upper airway. He was not a candidate for an instrumental assessment or trials of oral intake due to significant difficulty with secretion management and high aspiration risk.
Week 2
The RCP started spontaneous breathing trials with aerosol trach mask. The PMV was used both on and off the vent with total wear time or 2-4 hours twice a day. The SLP initiated expiratory muscle strength exercises in order to increase cough strength, increase airway protection and oropharyngeal strength. Initially this patient had difficulty coordinating lip seal and timing of breath for effortful exhalations required to participate in these exercises. The focus of therapy was on training the patient to coordinate lip seal and inhalation/exhalation through a semi-occluded airway (a straw). He was then transitioned to use of a threshold pressure device set at low pressure of 5 cmH20. The pressure threshold was increased as tolerated to the device maximum of 20 cmH20. He also continued use of a yankauer more independently to clear secretions orally and was able to maintain clear voicing for increased periods of time. As cognition improved, the patient participated in effortful swallow exercises with ice chips and saliva swallows.
Week 3
Patient was fully weaned from the ventilator and using the PMV during all waking hours. He demonstrated significant progress with indirect swallowing exercises and secretion management, therefore an instrumental swallow evaluation was initiated. A VFSS was conducted and all swallows were evaluated with the PMV in place. The results revealed aspiration of nectar thick liquids with a delayed cough and inability to clear the airway. Pureed and honey-thick liquid trials were tolerated without aspiration. There was moderate pharyngeal stasis with high risk of spillover aspiration. Therapeutic trials of puree and thickened liquids were initiated with SLP supervision.
Discharge
Secretion management improved sufficiently to allow decannulation before discharge from the LTAC facility. Due to continued oral and pharyngeal dysphagia, recommendations were made to continue therapeutic oral feeding trials and intense dysphagia rehabilitation at the skilled nursing facility.
Links of Interest
- Passy-Muir Continuing Education
- Principles of Deglutition (Relevant book chapter by Leder & Suiter referenced above)
About the Author
Julie Kobak, MA, CCC-SLP has been a speech language pathologist for 21 years and has worked with tracheostomized and ventilator dependent patients at both pediatric and adult rehabilitation hospitals, including the Cleveland Clinic Children’s Hospital for Rehabilitation. As Vice President of Clinical Education at Passy-Muir, Inc. she has lead the clinical education team in the development of numerous continuing education courses and products, including full day seminars, webinars, medical animation videos, and a quarterly clinical newsletter. As an expert in the field, Julie has provided numerous lectures and inservices on the topic of tracheostomy and Passy-Muir® Speaking Valves at hospitals and conferences nationally and internationally.
Additional contributions by:
Maribel Ciampitti, MS, CCC-SLP is highly experienced in the evaluation and management of communication and swallowing disorders in medically complex adult and geriatric patients requiring tracheostomy and ventilator support. Currently, Maribel works at Specialty Hospital, a long-term acute care facility and at UF Health in Jacksonville, FL, a level one trauma center. She has developed CEU courses and presented on the topic of Passy-Muir Valve application in the assessment and treatment of communication and swallowing related issues in the trach and vent dependent population.
Gail M. Sudderth, RRT has extensive experience in a variety of settings as a respiratory therapist. As lead therapist of a 32 bed intermediate care unit in a large teaching hospital, she was an integral member of the weaning team, and focused on the “hard to wean patient.” A recognized speaker, she has presented at state and national medical professional meetings in the United States and Canada on the topic of airway and ventilator management and the application of the Passy-Muir® Valve. She is currently a full-time clinical specialist for Passy-Muir Inc.
References
***There are 54 references in the above article. If you would like a full reference list, please click here





