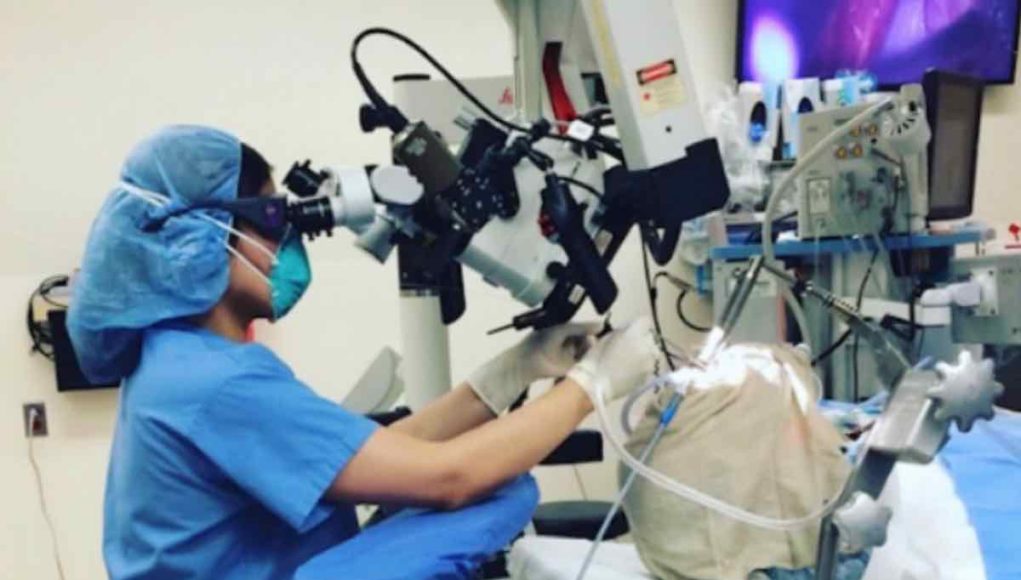
One of the most interesting aspects of working in the medical field is the opportunity to observe other professionals. Most of us only get to walk by each other in the hallway or read the name of a physician on an operative note in the electronic medical record.
Going into the operating room is not something most of us get a chance to do in our careers. So, I thought the Dysphagia Cafe readers might enjoy a behind the scenes look of a typical day of a Laryngologist. Dr. Inna Husain was gracious enough to give us that glimpse. Enjoy!
7:15 Arrive at the hospital.
I change my fabric mask for a surgical mask. I have my temperature taken and make my way to the staff elevators. I head up to the operating room floor.

7:30 Enter women’s locker room.
Here I change into hospital issued scrubs, don my trusty Danskos shoes, put on my selected scrub cap for the day, exchange my surgical mask for an N95 mask, and head over to pre-op holding. Pre-holding is where patients receive their IVs, confirmation of NPO status, meet the surgical and anesthesia team, review and sign consent for their surgery and the newest pre-operative check list item: obtain COVID testing. Since all the surgeries I perform involve the upper aerodigestive track, there is high risk of aerosolization if a patient is COVID-19 positive.

7:45 Although I have discussed the particular surgery with the patient previously, often during a clinic visit, I again review what the surgical plan for the day is, associated risks, benefits, and alternatives to the procedure, and review some post op instructions.
Key is to review strict voice rest instructions. This means reviewing what strict voice rest means and for how long I would like them to be on this rest (this is done during the preoperative clinic visit as well). Generally I do 1 week for phonomicrosurgical procedures. Patients are scheduled to start working with a voice therapist post op week 2 (after I have given medical clearance). Currently family members are no longer allowed in this area so I make sure I receive the family member’s name and number (if they will not be in the waiting room). This is also where I introduce my team to the patient. This usually includes an otolaryngology resident as well as a medical student on the service.
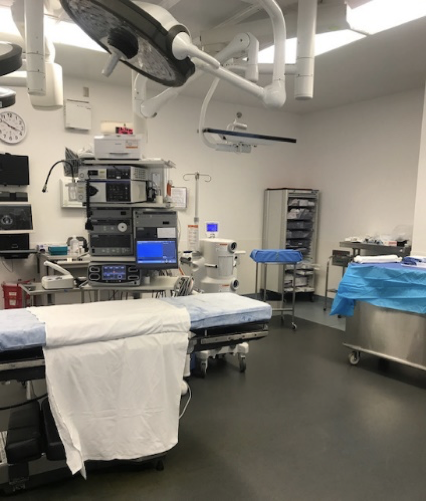


8:15 The operating room is ready and the room is “greened.”
This lets anesthesia know that it is ok to bring back the patient. The goal is for this to be done by the scheduled case time. This is most consistent for the first surgery of the day but often shifts as the day progresses. Once the patient enters the operating room, they are introduced to the nurse and scrub tech. Their ID is confirmed as is the consent for the surgery. The patient then transfers onto a narrow operating room bed. Often it is cold in the OR so we bring warm blankets for the patient.
8:30 The patient is placed under general anesthesia and intubated.
From there the patient is handed over to me, their surgeon. For laryngeal surgeries these days, we wear N95masks and eye protection (safety glasses or face shields). If using a laser, often we switch out the safety glasses for laser safety glasses. For phonomicrosurgery, I will gain view of the larynx with the rigid laryngoscope. I then bring in a microscope for a magnified view of the larynx. Micro-instruments are used to manipulate the tissues and perform the surgery.
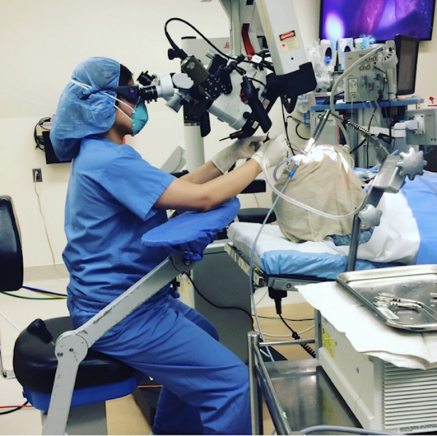
9:45 The surgery is completed and the patient is extubated.
I review the case description with the circulating nurse and we review the label for any specimens for the case. The patient is transferred back to their transport bed. We then take the patient to the post anesthesia care unit (PACU). Most of my surgeries are outpatient surgeries so once they have recovered in the PACU for a few hours, patients are discharged home.
10:00 As soon as we wheel the patient to the PACU and they are doing well, I like to go out to the waiting room and speak directly to the patient’s family.
I use this opportunity to review how the case went and review post op instructions. These instructions are also provided to the patient in written form as part of their discharge paperwork.
While the room is being cleaned and set up for the next case, I will dictate the just completed case. This is what is transcribed for the official operative report. My resident will do the discharge paperwork for the patient. We don’t have a lunch break so we use this time to have a snack, some water, or use the restroom.

This process is repeated for every case of the day. Changes are based on the type of surgery I am performing or the patient’s disease process. Some patients have straightforward airway needs, others are often complicated or difficult. Most cases hover around 1 hr of operating time, the open phonosurgeries often are closer to 2hrs. On average I have about 5 cases a day.
6:00pm I have finished dictating all cases and completing any outstanding orders.
I now return to the locker room to change, hang up my scrub cap, and head home to spend some time with my family. Surgery days can be long and exhausting but they are incredibly rewarding as well. I am humbled by the trust patients put in me to be their surgeon and I am honored to be their laryngologist.