Swallow studies in congenital aglossia

Congenital aglossia
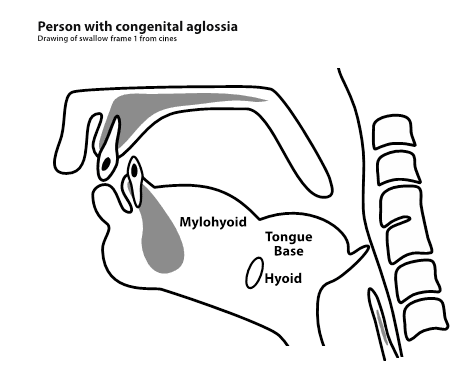
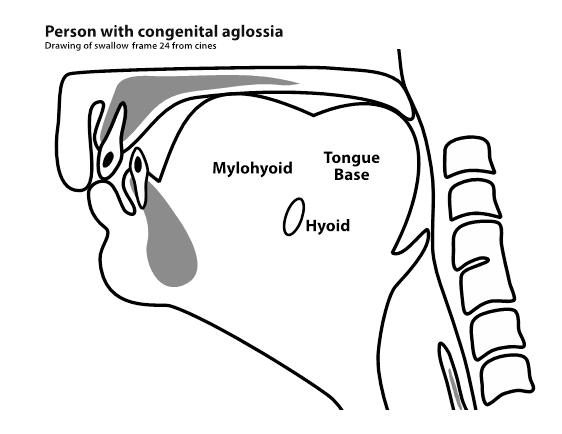
Congenital aglossia (CA) is a rare syndrome in which an individual is born without a tongue. It was de Jussieu in 1718 who first reported this syndrome. In the past 300 years 9 reports of isolated CA, without the presence of other syndromes or symptoms, have been reported.(1-17) (1,13,14,15 same case) (2,3,7 same case). There is a consensus among the former authors of congenital aglossia literature that the hypertrophied mylohyoid and tongue base act as a pseudo tongue, and that this pseudo tongue is successful in augmenting the person with congenital aglossias (PwCA) ability to speak and swallow in a perfectly functional and relatively normal fashion. In effect, the mylohyoid has hypertrophied from infant sucking as has the base of tongue, therefore providing compensation for loss of structure. There has been however only one attempt in the literature to describe or scientifically document the process of and anatomic structural relationships and physiologic associations that occur during swallow in the PwCA 2,3,7.
Modified Barium Swallow (MBS) in a case of congenital aglossia
In 2012, a modified barium swallow was administered to a 43 year old PwCA by Dr. Rebecca Leonard. The PwCA was not on a special diet and did not complain of needing any adaptive changes to meals. The results help us better understand the process of swallow with someone born without a tongue.
- General observations:
- At rest:
- evidence of absent tongue clearly apparent in oral cavity
- volume/bulk of base of tongue much greater
- hyoid appears to be elevated prior to swallow
- base of tongue in retracted position
- behaviors may be evidence of caution
- Small bolus sizes
- bolus material first arrives in pseudo-valleculae representing a transition between oral and base of tongue
- may contribute to prolonged oropharyngeal transit time
- no aspiration observed
- slight penetration noted that cleared with swallows
- larger bolus sizes appeared to be divided into two separate swallows
- At rest:
- Objective measures:
(for 20cc bolus, primarily).- Total pharyngeal transit prolonged (on the order of 1.2 secs)
- possibly because of slowed transition from oral to base of tongue
- prolonged times may be associated with increased effort
- Hyoid movement (1.62cm) and Hyoid-Larynx movement (1.28cm) were generally appropriate
- Possibly because the hyoid was in an elevated position to begin with, we expect it to appear somewhat reduced as compared to normal.
- Pharyngeal Constriction Ratio, wnl (.06)
- Ratio of the pharyngeal area with a 1cc bolus held in the oral cavity, to the same area measured at the point of maximum constriction during the swallow.
- Airway closure delayed relative to opening of PES.
- Typically, the airway (as determined by epiglottic-arytenoid closure of the laryngeal vestibule) closes before arrival of the bolus at the PES and, in our normal subjects, was never more than .1 sec later than PES opening.
- Subject’s closure times were sometimes more delayed; however, and though this is a risk factor for aspiration, it was not observed
- PES opening was reduced (on the order of .50+cm as opposed to the more typical .8-.9 for a 20cc bolus
- subject swallowed boluses in piecemeal fashion
- PES opening is directly related to bolus volume, so this may not be surprising. She may have a small web, but her opening in anterior-posterior view was wnl.
- Typically, the airway (as determined by epiglottic-arytenoid closure of the laryngeal vestibule) closes before arrival of the bolus at the PES and, in our normal subjects, was never more than .1 sec later than PES opening.
- Total pharyngeal transit prolonged (on the order of 1.2 secs)
A second MBS was completed on the same PwCA in 2013 and was interpreted by Angela Mandas, MA and Dr. Shelley Von Berg.
ANGELA MANDAS, M.A.
- Thin liquids –
- 1 tablespoon of liquid barium
- Client presented with good labial seal.
- As the bolus enters mouth
- hyoid moves superiorly and anteriorly
- mylohyoid simultaneously elevates and velum meets mylohyoid while closing off the nasopharynx
- swallow is swift and epiglottis tilts over laryngeal vestibule
- no evidence of penetration or aspiration noted
- one swallow was observed with no follow up dry swallows needed to clear the bolus.
- 1 tablespoon of liquid barium
- Nectar liquids
- 1 tablespoon of nectar thick barium
- oral phase characterized by identical movement seen with thin liquids with exception of 4 swallows needed to clear bolus.
- 1 tablespoon of nectar thick barium
- Soft solids
- client given teaspoon of applesauce impregnated with barium
- oral phase characterized as displaying 6 movements myohyoid and teeth to masticate applesauce to propel bolus as single unit
- oral transport required 2 separate elevations of myohyoid and velum to propel bolus posteriorly. Three dry swallows observed post bolus swallow. No misdirection of swallow noted.
- client given teaspoon of applesauce impregnated with barium
- Solids
- Client given graham cracker with barium paste
- oral phase consisted of 10 movements of mastication to prepare bolus for swallowing.
- client tilted chin superiorly during oral transport to pharynx.
- one dry swallow noted post bolus swallow.
- oral phase consisted of 10 movements of mastication to prepare bolus for swallowing.
- Client given graham cracker with barium paste
SHELLEY VON BERG, PhD.
- Subject tilts up anterior mandible to swallow. Perhaps assisting propulsion of liquids to posterior oral cavity.
- Soft solids:
- entire mandible appears to fill up maxillary space so there is close contact with mylohyoid and hard palate.
- possibly to allow mylohyoid contract to keep the bolus at center of oral cavity during mastication and prevent slippage into sulci.
- mandibular positioning would also help squeeze bolus along hard palate (stripping motion) for oral phase of swallow to posterior oral cavity, where tongue base can take over.
- entire mandible appears to fill up maxillary space so there is close contact with mylohyoid and hard palate.
- Solids:
- Subject tips her head back (hyperextends) for the oral prep and oral transit phases of swallow. Same behaviors as observed for soft solids.
Articulatory variables of pseudo-tongue, mandible and hyoid
In a publication in progress (18) the authors studied positional movements of the PwCA pseudo-tongue, (mylohyoid and base of tongue), mandible and hyoid and found that the pseudo tongue had various and often independent relationships with mandibular and hyoid bone movements during oral saliva swallow and speech. The highly predictable correlations of muscles for deglutition and speech suggest that this PwCA essentially ‘bootstrapped’ muscular actions (and limitations therein) developed for deglutition and used them to buttress speech and resonance as she matured. These actions are quite different from those of individuals with a tongue, who recruit a variety of muscles for the diverse acts of speaking and swallowing.
The authors suggested that the compensatory strategy of “bootstrapping” for speech should be adapted by speech language pathologists when working with individuals with congenital or surgical oral-facial anomalies that involve the loss of or damage to the tongue structure. Focusing on that act of sucking, as in the case of this PwCA, could potentially activate compensatory muscles such as the mylohyoid, and cause them to develop in a hypertrophic manner, which would then serve as articulatory structures for the development of intelligible speech.
References
- Allison, G. R., Salibian, A. H., McMicken, B., & Shoup, J. E. (1987). Adaptive mechanisms of speech and swallowing after combined jaw and tongue reconstruction in long-term survivors. American Journal of Surgery, 154, 419-422.
- Ardran, G.M., Beckett, J.M. & Kemp, F.H. (1956). Aglossia congenital. Archives of Disease in Childhood, 400-407.
- Ardran, G.M., Beckett, J.M. & Kemp, F.H. (1964). Aglossia congenita. Archives of Disease in Childhood, 39, 389-392.
- De Jussieu, A. (1718). Observations sur la maniere donc une fille sans langue s’acquitte des functions qui dependent de cet organe. [Observations of the manner in which a woman with no tongue accomplishes the functions that depend on that organ.] Memoires of l’Academie Royale des Sciences de Paris, 6-16.
- Eskew, H.A. & Shepard, E.D. (1949). Congenital aglossia. American Journal of Orthodontics, 122(4), 116-119.
- Farrington, R.K. (1947). Aglossia congenita; report of a case without other congenital malformations. North Carolina Medical Journal, 8(1), 24-26.
- Fulford, G.E. & Kemp, G.M.A. (1956). Aglossia congenita. British Medical Journal, 31(159), 400-407.
- Goto, S., Tanaka, S. & Iizuka, T. (1991). A case report of congenital aglossia. Aichi Gakuin Dental Sciences, 4, 7-14.
- Higashi, K. & Edo, M. (1996). Conductive deafness in aglossia. Journal of Laryngology and Otology, 110, 1057-1059.
- Hiiemae, K. M., Palmer, J. B., Medicis, S. W., Hegener, J., Jackson, B. S., & Lieberman, D. E. (2002). Hyoid and tongue surface movements in speaking and eating. Archives of Oral Biology, 47, 11–27.
- Khalil, K.C., Dayal, P.K., Gopakumar, R., & Prashanth, S. (1995). Aglossia: a case report. Quintessence International. 26(5), 359-360
- Kuroda, T. & Ohyama, K. (1981). Hypoglossia: case report and discussion. American Journal of Orthodontics, 79, 86-94.
- McMicken, B., Vento-Wilson, M., Von Berg, S., Iskarous, K., Kim, N., Rogers, K., & Young, S. (2013). Semantic and phonemic listener confusions in a case of isolated congenital aglossia. Communications Disorders Quarterly, 35, 74–83. doi:10.1177/1525740113504383.
- McMicken, B., Von Berg, S., & Iskarous, K. (2012). Acoustic and perceptual description of vowels in a speaker with congenital aglossia. Communications Disorders Quarterly, 34, 38–46.
- McMicken, B., Vento-Wilson, M., Von Berg, S., Rogers, K. (2014). Cineradiographic examination of articulatory movement of psedo-tongue, hyoid, and mandible in congenital aglossia. Communications Disorders Quarterly, doi: 10.1177/1525740114523310.
- Rasool, A., Zaroo, M.I., Ani, A.H., Darzi, M. A., Bashir, S.A., Biji, A.H., & Rashid, S. (2009). Isolated aglossia in a six-year-old child presenting with impaired speech. Cases Journal, 2(7926), doi: 10.4076/1757-1626-2-7926.
- Salles, F., Anchieta, M., Costa Bezerra, P., Torres, M. L., Queiroz, E., & Faber, J. (2008). Complete and isolated congenital aglossia: Case report and treatment of sequelae using rapid prototyping models. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontics, 105, e41–e47.
- McMicken, B., Von Berg, S., Wang, L., Kunihiro, A., Vento-Wilson, M., Rogers, K. (2015) A Comparison of Speech and Oral Swallow Movement in Congenital Aglossia. Submitted to Journal of In’t Rehab.